Introduction
Horner’s syndrome, also known as oculosympathetic paresis, is a clinical condition characterized by signs affecting the ipsilateral face and eye. First described in 1869 by Johan Friedrich Horner, it is characterized by the presence of ptosis, miosis, and anhidrosis, although the latter is frequently absent.
The pathophysiology of Horner’s syndrome involves a lesion in any of the three neurons of the sympathetic nervous system. This can occur at the central level (hypothalamus), the spinal level (C8-T2), or the postganglionic level (superior cervical ganglion). The sympathetic fibers travel with the brachial plexus and synapse in the superior cervical ganglion before innervating the Müller’s muscle (responsible for eyelid elevation) and the iris dilator muscle.
The diagnosis of Horner’s syndrome can be made based on the clinical features or confirmed with the cocaine test. In this test, two drops of 4% cocaine are instilled in each eye, and the amount of anisocoria is measured after 45 min. A positive test is indicated by an increase in anisocoria > 1 mm1.
When Horner’s syndrome is caused by local anesthetics, the underlying mechanism involves the diffusion of the anesthetic agent into the paravertebral space, leading to paralysis of the ipsilateral sympathetic cervical chain (stellate ganglion)2. Regional anesthesia techniques commonly associated with Horner’s syndrome include the interscalene block and the supraclavicular block, with reported incidences ranging from 4 to 37.5%3,4.
This case report presents a pediatric patient who developed Horner’s syndrome following a supraclavicular block for the reduction of an elbow fracture.
Case report
A 10-year-old healthy male patient, classified as American Society of Anesthesiologists physical status I, was scheduled for reduction and osteosynthesis of a right humerus fracture. The procedure was to be performed under sedation and a supraclavicular ultrasound-guided brachial plexus block. The patient received a continuous intravenous infusion of Hartmann’s solution for medication administration and was monitored with standard non-invasive monitoring including electrocardiogram, non-invasive blood pressure, and pulse oximetry (SpO2).
For the supraclavicular block, the patient was premedicated with fentanyl 25 μg and midazolam 3 mg. The neck was prepped with Chloraprep®, and a 10-12 MHz linear ultrasound probe (Sonosite P15000-63 Edge Portable Ultrasound System) was placed in the right supraclavicular area under sterile conditions. The subclavian artery was identified, and a 50 mm Stimuplex needle was inserted into the corner pocket. Local anesthetic, ropivacaine 0.2%, was injected at a volume of 7 mL (14 mg). Throughout the procedure, which lasted 120 min, the patient’s vital signs remained stable. Anesthesia was maintained with a propofol infusion at a rate of 30-50 μg/kg/min, and supplemental oxygen was provided through nasal cannula at a flow rate of 3 L/min.
Following the procedure, the patient was transferred to the post-anesthesia care unit (PACU) without any respiratory or hemodynamic instability. On re-evaluation in the PACU, Horner’s syndrome was observed (Fig. 1). However, there were no other side effects, including pulmonary, ventilatory, nor neurologic issues. The patient and his parents were informed that Horner’s syndrome is a known potential side effect of supraclavicular blocks and that the condition is typically transient. The anisocoria resolved completely within 8 h without any residual effects (Fig. 2).
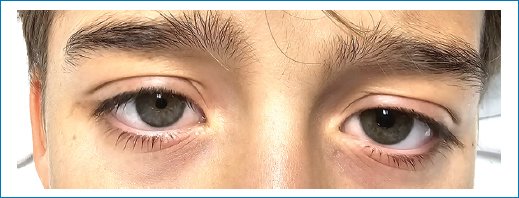
Figure 1. Horner’s syndrome.
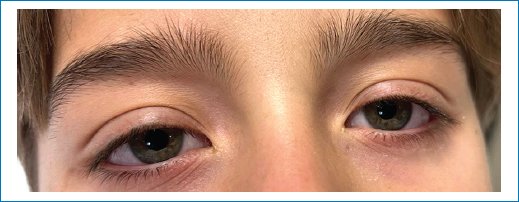
Figure 2. Complete recovery 8 h later.
Discussion
To mitigate the risk of this complication, Flores et al.5 recommends administering no more than 5 mL of local anesthetic to prevent its spread into the deep neck compartments. In addition, needle placement should be targeted at the superior pole of the thyroid gland (C4 level). Finally, proper injection depth is crucial. In this case, 7 mL of local anesthetic was used, which may explain the occurrence of Horner’s syndrome.
While retting6 reported a 100% correlation between Horner’s syndrome and alterations in hemidiaphragmatic movement, our patient did not exhibit any such complications.
Therefore, although Horner’s syndrome is a known benign side effect of regional anesthesia techniques, it can be uncomfortable for patients. It is essential to inform and reassure patients about this condition and its typically transient nature. Finally, it is essential to monitor patients closely in the PACU for any signs of neurological deficits or other complications. Early recognition and prompt intervention can help minimize morbidity. Especially since the differential diagnosis that comes with Horner’s syndrome can be of great clinical relevance.
Conclusion
Horner’s syndrome is a rare but recognized complication of brachial plexus blocks, particularly when local anesthetic spreads to the cervical sympathetic chain. Although it is typically benign and self-limited, its appearance may cause concern for both patients and clinicians. Awareness of this potential effect, cautious administration of minimal effective anesthetic volumes, and the use of real-time ultrasound guidance are key to reducing its incidence. Early recognition, patient reassurance, and appropriate monitoring ensure optimal outcomes and reinforce the safety of regional anesthesia techniques in pediatric patients.
Funding
The authors declare that they have not received funding.
Conflicts of interest
The authors declare no conflicts of interest.
Ethical considerations
Protection of humans and animals. The authors declare that no experiments involving humans or animals were conducted for this research.
Confidentiality, informed consent, and ethical approval. The authors have followed their institution’s confidentiality protocols, obtained informed consent from the patient’s parents, and received approval from the Ethics Committee. The SAGER guidelines were followed according to the nature of the study.
Declaration on the use of artificial intelligence. The authors declare that no generative artificial intelligence was used in the writing of this manuscript.
